Neurological Examination Channels:
Univ. of Nebraska Neurological Examination - Adult
One of the best websites/channels, detailing all you need to know about neurological examination by Dr. Paul Larson.
Univ. of Nebraska Neurological Examination - Pediatric
One of the best websites/channels, detailing all you need to know about neurological examination by Dr. Paul Larson.
NeuroRadiology
Neuroradiology Advanced - LNR Course
All what you need to know about neuroradiology
More directed to PGY3/4
Grand Rounds
UA Neurology Grand Rounds
University of Arizona, Neurology Department grand rounds iTunes U channel.
You will need to download iTunes U then search for Neurology grand rounds
Audio/Video Lectures
Neurology - Podcast
Weekly podcast of content from Neurology®, the official journal of the American Academy of Neurology.
Continuum Audio Digest
If you don't have the time to read, then you can listen. Listen to lectures highlighting the important parts in the bi-monthly Continuum.
Free access for junior members, follow the link for more details.
Clinical Neurology Courses
Coursera - Medical Neuroscience, Duke University
An introduction of Neuroscience from Duke university. Starts with neuroanatomy and takes you through the physiology and how the brain works.
MDS Fundamentals Course
Movement disorders fundamental course by MDS (Movement Disorders Society)
Membership of MDS is free for neurology residents. Click here to proceed with free subscription.
Harvard University Fundamentals of Neuroscience
Fundamentals of Neuroscience, a free online course sponsored by Harvard School of Medicine
EEG Courses
USF EEG Fellowship Course
Online EEG course by USF and EEGCare. Usually held July-December.
About 3000 for physicians - 1500 for residents
NeuroIimmunology Resources
USF EEG Fellowship Course
Online EEG course by USF and EEGCare. Usually held July-December.
About 3000 for physicians - 1500 for residents

























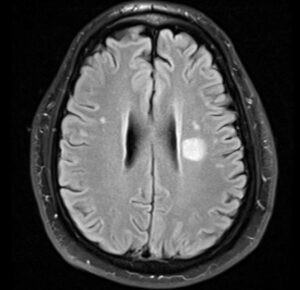
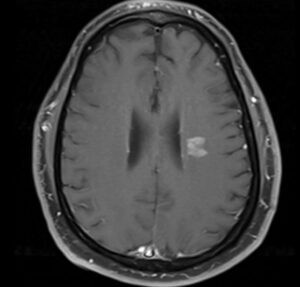

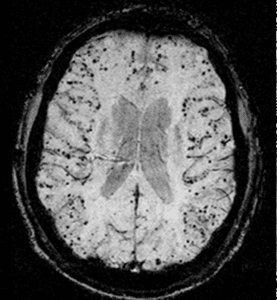
![Cerebral_amyloid_angiopathy_(CAA)-MRI By Marvin 101 [CC BY 3.0 (https://creativecommons.org/licenses/by/3.0)], from Wikimedia Commons](https://neurologyresidents.com/wp-content/uploads/bb-plugin/cache/Cerebral_amyloid_angiopathy_CAA-MRI-landscape-feda5685e321ed812b6f6b2e76ed4b88-5b82dfebd5f4b.png)

